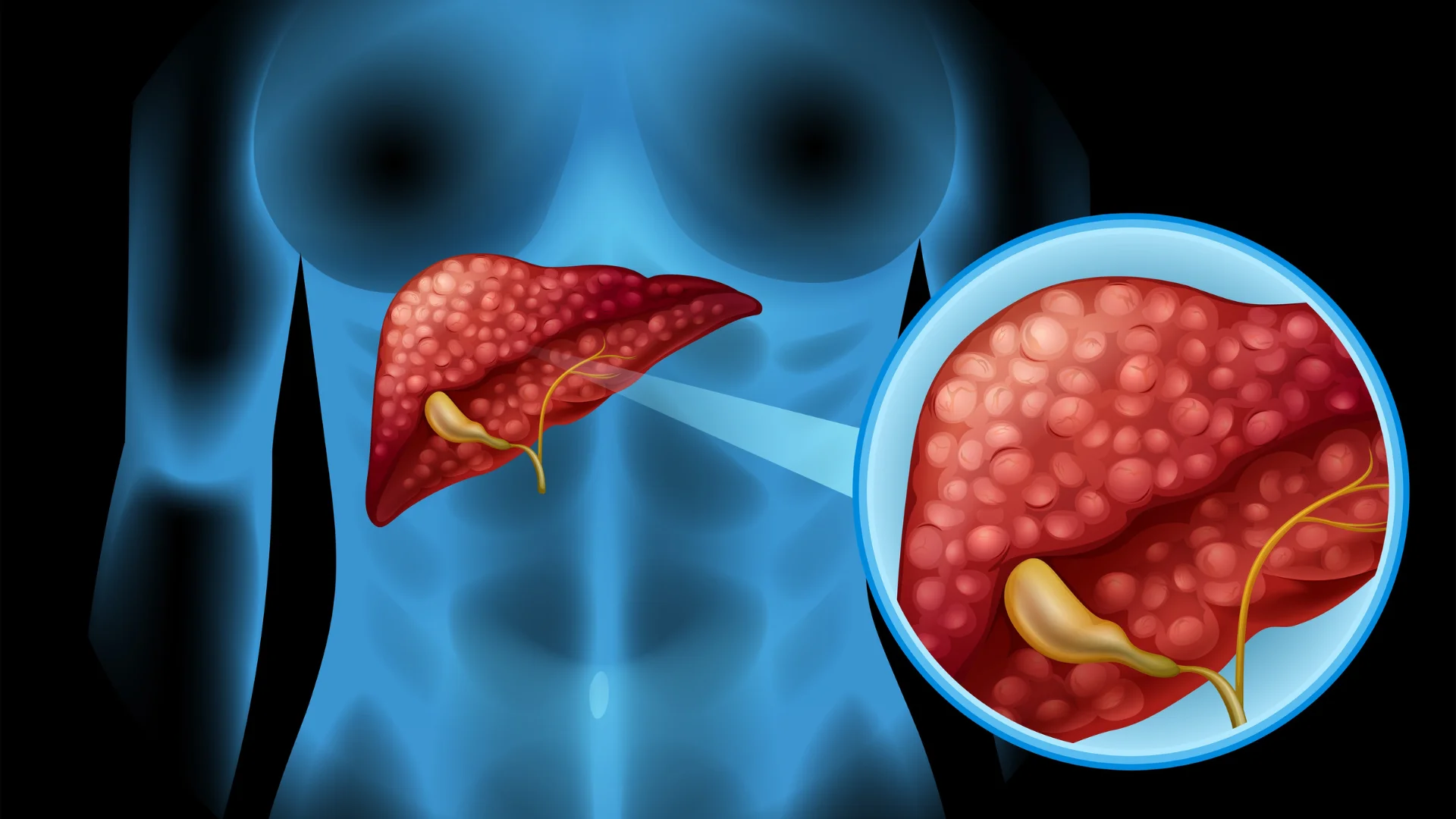
Liver cirrhosis is a long-term condition where the liver becomes badly scarred. Healthy liver cells slowly die and are replaced with hard scar tissue. Over time, this scarring makes it difficult for the liver to do its important jobs such as cleaning the blood, helping digestion, storing nutrients, and controlling bleeding.
In Uganda, liver cirrhosis is common due to hepatitis B, hepatitis C, alcohol use, and other medical conditions. Many people only realise they have cirrhosis when serious complications appear. Early detection and proper care can slow the disease and prevent life-threatening problems.
If you are worried about liver disease or have been told you may have cirrhosis, Hope Plus can connect you to a licensed healthcare provider within minutes. A provider can review your symptoms, interpret your results, and guide you on the next steps, including referral to the right hospital. Learn more here: https://hope.co.ug/plus/
Key Takeaways
- Liver cirrhosis is permanent scarring of the liver.
- In Uganda, common causes include hepatitis B, hepatitis C, and alcohol use.
- Early stages may have mild symptoms, but advanced stages can be life-threatening.
- Patients are referred to regional hospitals or higher-level facilities for specialist care.
- Treating the cause and preventing complications can improve survival.
What Happens in Liver Cirrhosis?
Cirrhosis develops slowly. At first, the liver may become enlarged. Later, it may shrink as scarring worsens.
When cirrhosis becomes severe and causes complications, it is called decompensated cirrhosis. This means the liver can no longer cope.
Serious complications include:
- Ascites, which is fluid collecting in the abdomen
- Bleeding from swollen blood vessels in the oesophagus
- Confusion due to toxin build-up, called hepatic encephalopathy
- Jaundice, which is yellowing of the eyes and skin
Causes of Liver Cirrhosis in Uganda
Cirrhosis can be caused by:
1. Infections
- Chronic hepatitis B
- Hepatitis C
- Hepatitis D
2. Alcohol and Toxins
- Long-term heavy alcohol use
- Certain medicines such as methotrexate, isoniazid, and methyldopa
- Toxic substances
3. Fatty and Infiltrative Liver Diseases
- Non-alcoholic fatty liver disease
- Wilson’s disease
- Haemochromatosis
4. Iron Overload
This can happen in people who receive frequent blood transfusions, such as some patients with sickle cell disease.
5. Autoimmune Conditions
Chronic autoimmune hepatitis.
6. Bile or Blood Flow Problems
- Primary biliary cirrhosis
- Chronic heart failure
- Budd Chiari syndrome
Sometimes, no clear cause is found. This is called idiopathic cirrhosis.
Symptoms of Liver Cirrhosis
Early Symptoms
In early stages, symptoms may be mild:
- Fatigue
- Weight loss
- Poor appetite
- Nausea and vomiting
- Signs of malnutrition
- Reduced sexual desire
- Enlarged liver at first
Later Symptoms
As the disease worsens:
- The liver may become smaller
- Blood vessels may appear clearly on the abdomen
- The spleen may enlarge
- The abdomen may swell with fluid
- Legs may swell
- Yellowing of the eyes and skin
- Vomiting blood from ruptured veins in the oesophagus
- Confusion or unusual behaviour
Stages and Risk
Cirrhosis progresses in stages.
In early compensated cirrhosis, there are no major complications and survival is better.
In decompensated cirrhosis, complications such as ascites, bleeding, kidney failure, infection, liver cancer, and encephalopathy increase the risk of death significantly.
This is why early treatment and monitoring are very important.
How Liver Cirrhosis Is Investigated in Uganda
Patients are referred to a regional hospital or higher-level facility for specialist care.
Investigations may include:
Blood Tests
- Haemoglobin and blood film
- White blood cell count
- Platelet count
- Prothrombin time and INR to assess clotting
- Hepatitis B, C, and D tests
- HIV test
- Liver function tests
- Alpha fetoprotein to screen for liver cancer
An APRI score greater than 2 suggests cirrhosis.
Stool and Urine Tests
These help assess overall health and rule out other conditions.
Abdominal Ultrasound
An ultrasound is done to:
- Assess liver size and texture
- Detect fluid in the abdomen
- Look for liver masses
- Assess spleen size
Endoscopy
If bleeding is suspected, a camera test called endoscopy is performed to look for enlarged veins in the oesophagus.
Liver Biopsy
In some cases, a small sample of liver tissue is taken to confirm the diagnosis.
Management of Liver Cirrhosis in Uganda
Patients should be managed at a regional hospital or higher-level facility under specialist care.
Step 1: Treat the Cause
- Alcohol must be completely stopped.
- If chronic hepatitis B is present, antiviral treatment is started.
- Specific treatment is given depending on the cause.
- Herbs and self-medication are strongly discouraged.
- Medicines are only used after prescription by a qualified health worker.
- Proper nutrition support is provided.
Step 2: Prevent Disease Progression
- Regular monitoring of liver function.
- Vaccination and infection prevention where appropriate.
- Close follow-up visits.
Step 3: Manage Complications
Healthcare providers manage complications such as:
- Ascites, where medicines are given and fluid may be drained if necessary.
- Encephalopathy, where medications are given to reduce toxin build-up.
- Bleeding varices, where emergency treatment and endoscopic procedures are performed.
Hospital admission is often required for severe complications.
Prevention of Liver Cirrhosis
You can reduce your risk by:
- Getting tested and treated early for hepatitis B and C.
- Avoiding excessive alcohol use.
- Avoiding herbal medicines and unprescribed drugs.
- Seeking medical care for chronic conditions like heart failure.
- Ensuring safe blood transfusions and sterile medical procedures.
Frequently Asked Questions
1. Can liver cirrhosis be cured?
The scarring cannot be reversed once it is severe. However, treating the cause can stop or slow further damage.
2. Is cirrhosis the same as liver cancer?
No. Cirrhosis is scarring of the liver. However, cirrhosis increases the risk of developing liver cancer.
3. Can I live a normal life with cirrhosis?
If diagnosed early and properly managed, many people live for years with good quality of life. Advanced stages require close monitoring.
4. Should I stop alcohol completely?
Yes. Even small amounts of alcohol can worsen liver damage in cirrhosis.
5. Are herbal remedies safe for liver disease?
No. Many herbs can worsen liver damage. Only medicines prescribed by a qualified health worker should be used.
6. What should I eat if I have cirrhosis?
Healthcare providers usually recommend a balanced diet with adequate protein and calories. In some cases, salt intake may be reduced if there is swelling.
7. When should I go to hospital urgently?
Seek emergency care if there is vomiting of blood, severe abdominal swelling, confusion, yellowing of the eyes, or reduced urine output.
If you suspect liver disease or have been told you have cirrhosis, early medical care can save your life. Do not delay seeking professional help.